Types of Birth Control: Is Yours Effective Enough?
Here is everything you need to know about your post-Roe birth control options and which are the most effective.
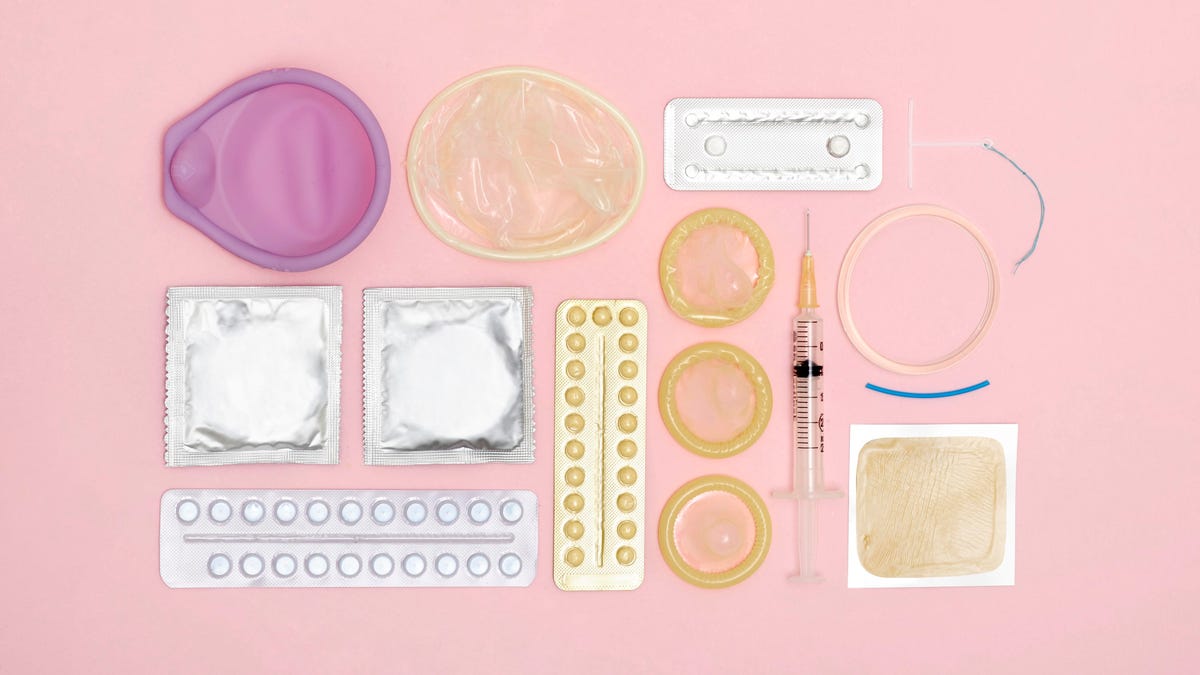
In our post-Roe world, you may be turning to friends and the internet to learn what your birth control options are. You might be wondering, "Which birth control methods are right for me? Which are the most effective?" And, as of recently, "Will I continue to have access to birth control?"
While some over-the-counter birth control options, such as condoms, are most likely to always stay available, there is concern around access to other methods of contraceptives.
Read more: Could a Post Roe v. Wade World Impact Your Access to Birth Control?
If you are wondering if your form of birth control is effective enough, here are some of the most successful (and least) ways to prevent pregnancy.
What is birth control?
Birth control prevents pregnancy from taking place. Contraceptives can take many forms, such as a pill, shot, implant or vaginal ring, and some require medical procedures like tubal ligations and vasectomies. The main goal of any birth control method is to prevent sperm from coming in contact with an egg.
Birth control is different from emergency contraceptives, like Plan B, which help prevent an already fertilized egg from implanting in the uterus and stop ovulation. The abortion pill, which terminates pregnancies, isn't considered birth control either. Birth control is used before and during sex, while emergency contraceptives are used within 120 hours after unprotected sex or failed contraceptives.
It is important to note that not all birth control protects against sexually transmitted diseases. The only methods that can protect against STDs are male and female condoms. However, they can only protect you from diseases transmitted by bodily fluids or skin contact, but only where skin is covered by the condom.
How to access birth control
Some access to non-hormonal birth control is fairly easy. For example, condoms can be found almost anywhere: drug stores, gas stations or grocery stores. Spermicide is also sold in these same places.
However, hormonal birth control is harder to obtain. The pill, an intrauterine device or other hormonal birth control methods must be prescribed by a doctor, like your gynecologist. Seek your healthcare provider, local health facility or university doctor to learn about your options.
A lot of times, insurance will cover or lower the cost of your visits and prescriptions.
What are the different types of birth control?
Here are some of the types of birth control available and the effectiveness of each birth control option.
The pill
The oral birth control pill contains up to two hormones -- estrogen and progestin. You can find two types of pills, combination and progestin-only. Combination pills contain estrogen and progestin. The pill is prescription-only, and your doctor will determine which pill is best for you based on your medical history and conditions.
The pill works by utilizing the hormones to stop ovulation (the release of an egg), thus preventing sperm from connecting with an egg. The pill also thickens the cervix mucus, making it harder for sperm to travel to an egg. This method requires daily pills at the same time each day for maximum effectiveness.
Shot
The birth control shot, also known by its brand name, Depo-Provera, is a hormonal injection. Each injection contains the hormone progestin, and the method requires a shot every three months. You can receive this contraceptive through your doctor.
The shot works similarly to other hormonal methods. Progestin prevents ovulation and thickens the cervix mucus. Sperm have a harder time connecting with an egg.
Implant
A birth control implant (such as the name brand, Nexplanon) is inserted into the skin of the upper arm. The thin, flexible, rod-like structure releases the hormone progestin into the body. It is effective for up to three years. Receive an implant from your doctor.
Implants work like any other hormonal birth control method. Progestin prevents ovulation and thickens the cervix mucus. The implant can be removed by a doctor before the five years is up.
IUD
An IUD is a small 'T'-shaped device made of plastic that is inserted into the uterus. There are two types of IUDs: hormonal and copper. The hormonal IUDs (like Mirena and Kyleena) can last anywhere from three to seven years. The copper IUDs (Paragard) can last for up to 12 years, though 10 is usually recommended. Receive this contraceptive from your doctor or gynecologist.
IUDs work by interrupting the movement of sperm in their search for an egg. The copper IUDs repel sperm, and the hormonal IUDs release progestin. Both types of devices can also be used as an emergency contraceptive if inserted within five days of unprotected sex.
Diaphragm
A diaphragm is similar to a menstrual cup. It is shaped like a dome, it is bendable, often made of silicone and inserted into the vagina. After obtaining a prescription from your doctor, you can buy a diaphragm at a pharmacy or drugstore. You can visit a gynecologist to be fitted for the correct diaphragm, and the doctor will demonstrate how to insert it. Your diaphragm should be replaced every two years and used in combination with spermicide to be the most effective.
This device prevents pregnancy by covering the cervix and blocking sperm from entering it. The added spermicide also stops sperm from moving toward the egg.
Spermicide
Spermicide, often a gel or cream, is inserted into the vagina before sex. The chemicals in spermicide hinder sperm from being able to move enough to find an egg. Spermicide is more effective when paired with another birth control method such as the pill or intrauterine device. You can find spermicide over-the-counter in most drugstores or pharmacies.
Make sure to always read the directions on the spermicide; some are not supposed to be used with latex products (such as condoms).
Contraceptive sponges
Like a diaphragm, birth control sponges are inserted into the vagina right before sex. The small, round sponge part blocks the cervix during intercourse. Unlike a diaphragm, a sponge already contains spermicide and you do not need to visit your doctor to get one.
The spermicide and the sponge block sperm from reaching the uterus and connecting with an egg. It can be paired with or without a condom. Once the sponge is inserted, it protects you for 24 hours. After that, it needs to be replaced before having sex again.
Vaginal ring
A birth control vaginal ring is a small, flexible circle that is inserted into the vagina. Name brands of vaginal rings include NuvaRing and Annovera. One NuvaRing lasts about five weeks, and an Annovera ring lasts up to one year; take it out each month during your period. Visit your doctor for a prescription.
Both brands work by releasing both hormones estrogen and progestin -- which stops ovulation and increases cervical mucus. To be the most effective, a new ring must be inserted right on time.
Cervical cap
Similar to a diaphragm or a birth control sponge, cervical caps are inserted into the vagina and cover the cervix. It doesn't come with spermicide, so it needs to be used in combination with it to be more effective. You must leave a cervical cap inside the vagina after sex for at least six hours. After receiving a prescription, you can find a cervical cap at a pharmacy. Your doctor will also fit you for the right size.
A cervical cap with spermicide blocks sperm from entering the cervix and, thus, the uterus. It can be used again once it has been taken out and washed properly.
Withdrawal (Pull-out)
The pull-out method or "withdrawal" is when a person removes their penis from the vagina a few moments before ejaculation. This stops semen from ever entering the vagina. However, this method is tricky. If not timed correctly or if pre-ejaculation fluid (that may contain sperm) enters the vagina, there is a risk of pregnancy. Also, if this method is not paired with a condom, it can not protect against STDs.
Withdrawal is the most effective when combined with other methods such as condoms, vaginal rings or the pill.
Patch
A birth control patch attaches to a part of your body (upper arm, back or belly) and releases hormones into your body through the skin. The patch contains both estrogen and progestin hormones. Patches can only be prescribed to you by a doctor.
Both hormones work together to stop ovulation, increase cervical mucus and make it harder for sperm to reach an egg. You will need to change your patch every week, but on your period you won't wear one. Like with birth control pills, you need to put a new one on at the same time each week.
Condoms
Condoms are one of the most commonly used birth control methods. Male and female (internal) condoms are available, and both types of condoms block semen from entering the vagina. Male condoms can be made of latex, plastic or animal skin, and internal condoms are non-latex.
Each condom can only be used once, but male and internal condoms are the only methods that protect against STDs -- although animal skin condoms do not.
Sterilization
For anyone with a uterus and ovaries, tubal ligation is a surgical way of permanently preventing pregnancy. A vasectomy is a surgical method for people who produce sperm. Tubal ligation blocks fallopian tubes from releasing eggs, and a vasectomy blocks sperm from entering the semen.
Both procedures are permanent (but some vasectomies can be reversed). However, in rare cases, those who have had these procedures can still get pregnant or get someone pregnant.
Abstinence
Abstaining from sexual intercourse is the only way to completely prevent pregnancy.
Side effects of birth control
No birth control method is perfect, and each type has its risks. Each body is different and may react to forms of birth control differently. Consult your doctor to determine the best method of birth control for you.
Hormonal birth control
Because hormonal methods affect your hormones, the side effects can range from mild and unnoticeable to severe. While most of these hormonal methods are well tolerated, they can cause issues for some people that prevent them from using them.
For example, using hormonal birth control that contains estrogen can increase the risk of stroke in people who experience migraines with an aura. If that is the case for you, there are progestin-only options that don't increase stroke risk.
As always, you should consult a doctor before beginning any of these methods. Side effects of hormonal birth control like pills, IUDs, implants, shots, rings or patches include:
- Blood clots
- Migraines
- Pelvic inflammatory disease (PID)
- Weight gain
- Acne
- Nausea
- Mood swings
- Irregular periods
Non-hormonal birth control
Side effects of using condoms, diaphragms, sponges, spermicide, a copper IUD, a cervical cap or other non-hormonal methods include:
- Allergic reaction
- Irritation
- Dryness
- Toxic shock syndrome (although rare but serious)
- Burning
- Rash
- Pelvic inflammatory disease (PID)
- Longer and heavy periods with copper IUDs


