How some COVID vaccines may cause blood clots -- and what scientists are doing about it
Adenovirus vaccines developed by Johnson & Johnson and AstraZeneca have been associated with unusual blood clots in very rare cases.
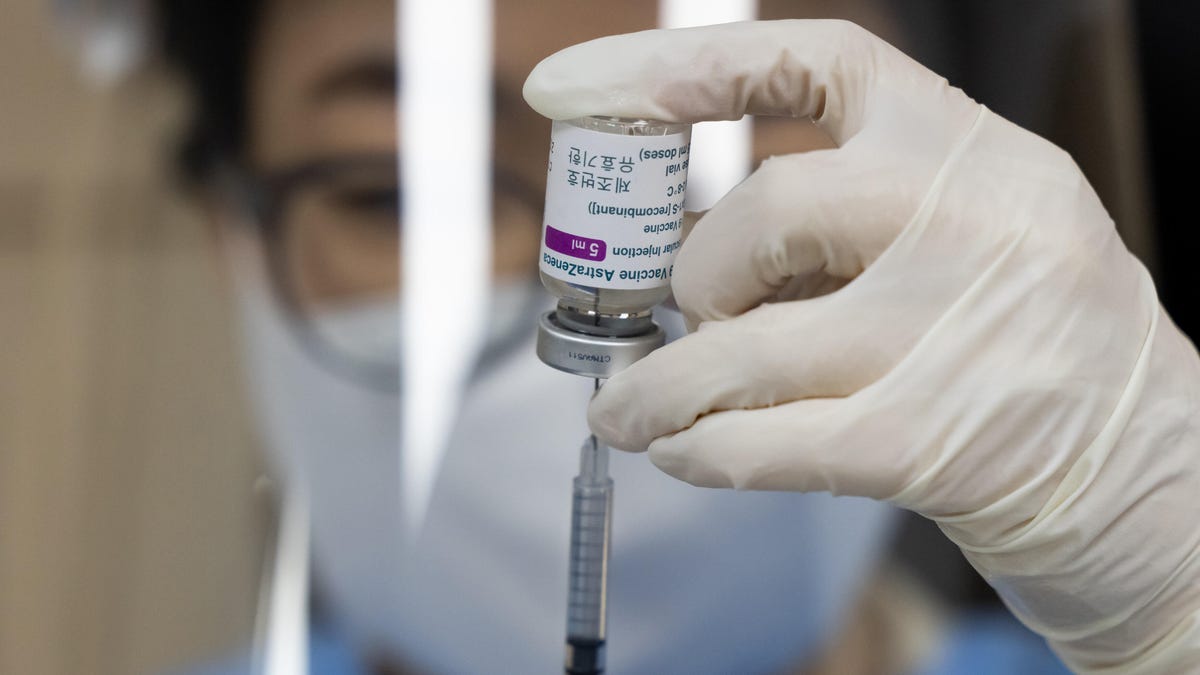
Blood clots have been classified as a very rare side effect of the AstraZeneca vaccine.
In the global race for a coronavirus vaccine, one group leaped ahead early. The team from Oxford University and British-Swedish biotech firm AstraZeneca first began injecting doses of their vaccine, now named Vaxzevria, into patients in April 2020.
The vaccine, which uses a reprogrammed chimpanzee virus, has been shown in large clinical trials to be safe and effective at preventing serious illness and death. It's now approved for use or emergency use in almost 100 countries and forms the backbone of the World Health Organization's COVAX initiative, which aims to provide equitable access to vaccines across the globe, opening up vaccine rollouts in dozens of low-income countries.
But it's suffered a number of setbacks. Miscommunications with the US Food and Drug Administration and dosing mistakes in clinical trials have eroded confidence in the shot, particularly in the US, where it's yet to be approved for use.
Its latest setback may be the biggest of them all. A spate of reports in February and March showed AstraZeneca's vaccine may be associated with a rare, sometimes fatal blood clotting condition. Instances of clotting were detected in a handful of European countries, including Austria, Denmark and Norway, and in late March, some began pausing the vaccine rollout while the European Medicines Agency investigated.
After a lengthy investigation and review, the EMA announced on April 7 that the clotting events should be listed as "very rare side effects" of the vaccine. The side effect has been given its own name: vaccine-induced immune thrombotic thrombocytopenia, or VITT.
As it stands, scientists aren't exactly sure how Vaxzevria causes the clots -- or even if the vaccine is the causative agent, though the link has become much more clear in recent weeks. The tiny numbers of affected patients, about four cases per million in the UK, seem to have a unique immune reaction that presents similarly to other known clotting conditions. This provides some clues as to how vaccination might cause these very rare events.
It also heralds potential clotting issues for the Johnson & Johnson vaccine, which uses the same technology. On April 13, the US FDA and the Centers for Disease Control and Prevention paused the rollout of J&J's vaccine to investigate rare clotting events in six women who had received the shot. Currently, the chance of experiencing the clotting side effect is less than one in a million for J&J and perhaps one in 100,000 for the Vaxzevria shot.
With both vaccines so intricately tied to returning to some semblance of normalcy, scientists must run a new race: unravel how the vaccines can disturb blood flow and learn how to manage the very rare side effects of vaccination.
How does clotting occur?
Blood is a complex milieu of cells and proteins. It carries oxygen around the body in a dense network of differently sized tubes, like veins and capillaries. It also circulates immune cells and signaling molecules, fighting off invading pathogens and cleaning up any microscopic mess.
Essentially, bodies are intricate plumbing networks of odd-shaped pipes.
Every now and then, a pipe might burst or leak. Fortunately, thanks to evolution, there's an army of plumbers waiting to plug the hole. Predominantly, these plumbers come in the form of platelets, specialized cell fragments that contain no DNA.
Anytime a leak occurs, platelets activate and stick together, plugging the hole, while simultaneously kicking off the "coagulation cascade" (coagulation is the process of liquid blood turning to a gel-like substance). The cascade involves a mix of blood proteins that help strengthen the plug. This is colloquially dubbed a clot and is a routine wound healing process that prevents us from bleeding to death when blood vessels are injured.
An artist's illustration of platelets (purple) travelling through the bloodstream.
But sometimes clots form in unusual places.
"A thrombosis is when a blood clot has occurred in the wrong place at the wrong time," says Vivien Chen, a blood specialist at the University of Sydney.
Platelets were discovered in 1882, by the Italian pathologist Giulio Bizzozero, so scientists have had over a century to tease out how they enable clots to form. They've also discovered a number of conditions that mess with platelet numbers, causing them to dip too low or rocket too high. Too many platelets is a bad thing because it may result in enhanced clotting. Too few platelets and you'll bleed more readily. We can measure platelet numbers with a simple blood test.
Thrombocytopenia is the term used to clinically define a low platelet count. It almost seems paradoxical, but the low platelet count can indicate increased clotting.
This is what can happen in VITT.
Can the AstraZeneca vaccine cause clots?
The AstraZeneca vaccine works by directing human cells to make tiny, harmless pieces of the coronavirus known as the spike protein. Usually, the coronavirus, or SARS-CoV-2, uses this spike to get inside human cells.
By making harmless pieces of the spike, the vaccine tells the immune system what the invader will look like, generating antibodies and priming the system in case you encounter the real thing.
To get the instructions into a human cell, where they can be read, AstraZeneca wraps them inside a different kind of virus, known as an adenovirus, in this case a chimp virus. The research team at Oxford and AstraZeneca removed most of the molecular machinery that allows the chimp adenovirus to replicate, essentially turning it into a courier that ferries spike protein instructions into our body.
Each shot is full of these couriers -- thousands of adenovirus particles ready to deliver instructions and prime the immune system. But the couriers could, potentially, be causing their own problems, interacting with the immune system in unexpected ways.
"Patients that developed thrombosis following vaccination appear to be predisposed [for currently unknown reasons] to have a strong immune reaction," says Jose Perdomo, a researcher in the Haematology Research Unit at the University of New South Wales.
In VITT, the plumbers are sent to work in the body's pipes, but there's no leak to speak of. They've been activated by the immune system.
Two studies, published in the New England Journal of Medicine on April 9, shows this very rare side effect resembles a clotting disorder known as heparin-induced thrombocytopenia, a condition that sometimes occurs when patients are put on a widely used, anti-clotting medication known as heparin.
A similar condition has been seen before
Heparin-induced thrombocytopenia, or HIT, is a diabolical disorder because it turns the medication against the patient. The drug is designed to reduce clotting, but in HIT, it actually seems to increase it.
That's partly due to a molecule known as Platelet Factor 4, which is released from activated platelets. When combined with heparin, PF4 can sometimes be a powerful clotting stimulator. Because these molecules circulate through the body, Perdomo says clots can appear in unusual locations, like the brain.
The incidence of HIT is as low as one in 500 in the general population, and it seems to affect women more than men but, Perdomo notes, "we don't understand why." One hypothesis is that females might mount a stronger reaction to immune complexes, he says, and another is that PF4 interacts more strongly with platelets in female patients.
A vial of heparin, a commonly used anticoagulant, sometimes described as a blood thinner.
It's an important note, because the clotting events seen so far with Vaxzevria and the J&J vaccine appear to be occurring more often in young women.
But, critically, VITT isn't HIT.
In the studies published April 9 in NEJM, the two research teams found that clinically, VITT has a similar profile to HIT -- but it's not identical. Patients with VITT hadn't been receiving heparin, so PF4 may be acting alone. "The syndrome is analogous to, but not exactly the same as, autoimmune heparin induced thrombocytopenia (aHIT)," Chen said.
The suggestion is that antibodies generated by the body after vaccination are causing increased clotting alone, just like in aHIT.
But scientists aren't yet sure exactly what the underlying mechanism is, or which molecule is responsible for forming these pro-clotting complexes. There's potential the adenovirus itself generates antibodies which bind PF4 without the need for heparin. Another theory is the adenovirus binds directly to platelets and activates them. "It's too soon to draw any firm conclusions," Adam Finn, professor of pediatrics at the University of Bristol, told the UK Science Media Centre.
How are scientists investigating the unusual clots?
Investigating the mechanism of action is a key next step.
"We have an understanding of how [the] process works, but in the case of the vaccine it's unclear how it's triggered," Perdomo says.
If the clotting condition is caused by a very rare reaction to the adenovirus used in Vaxzevria -- and, again, scientists aren't sure about this yet -- it could be problematic for other vaccines using adenoviruses, such as the Johnson & Johnson's and Russia's Sputnik V. (The Moderna and Pfizer vaccines use mRNA, a different technology.) Researchers have begun to see some extremely rare clotting cases during J&J's vaccine rollout in the US.
On April 13, the FDA and the CDC recommended the Johnson & Johnson vaccine rollout be paused "out of an abundance of caution." The FDA said it had received reports of six cases of rare clots out of more than 6.8 million administered doses of the vaccine in the US, a statistically minuscule risk. All cases occurred in women, and one patient died.
But there is good news. While investigating whether there is an underlying link between the vaccines and clotting could take several months, it's important to stress scientists understand how the immune system might cause these abnormal clotting issues -- and that makes them treatable. "Early diagnosis is allowing us to treat these patients," Chen notes.
A clear diagnostic pathway has been developed for patients who have received Vaxzevria and present with symptoms of VITT, with recommendations for the types of medications they should receive and those to avoid.
Another potential fix? Halving the dose of the vaccine. According to Science Magazine, Andreas Greinacher, a clotting expert at Germany's University of Greifswald and author of one of the NEJM studies, suggests this potentially simple remedy might trigger a mild immune response without compromising the vaccine's effectiveness. The approach is yet to be tested.
Weighing risks and benefits
The COVID-19 vaccines that are currently available across the world have been shown to prevent serious illness and death. They don't all work the same way. But no matter the vaccine technology, the end result of extensive clinical trials has been the same: the immune system is primed and ready to fight off the coronavirus and prevent disease.
The very rare side effect of the AstraZeneca shot -- and, potentially now Johnson & Johnson -- does require investigation, but this is a routine step during vaccination rollouts. The FDA, for instance, follows serious side effects from vaccines with a surveillance program known as the Vaccine Adverse Event Reporting System.
Many national health bodies, including the European Medicines Agency and the WHO, continue to champion the safety profile of the AstraZeneca vaccine, though some countries are taking a cautious approach in rolling the jab out. Several European nations and the UK have completely paused or revised advice on which age groups should receive Vaxzevria. For instance, while Australia is advising those under 50 should receive a different vaccine, the UK set the age at 30. Each nation has to weigh up the risk of contracting COVID-19 and the risk of these very rare side effects in their population. "Decisions like these are political, social, ethical as well as evidence-based," says Jane Williams, a health ethicist at the University of Sydney, Australia.
But the differing recommendations can be confusing, highlighting the need for national governments to communicate transparently with the public. There are concerns that pauses could lead to increased vaccine hesitancy, according to Ross Gordon, a behavioral scientist at the Queensland University of Technology in Australia.
Explaining the context around each strategy will be paramount to preventing a dip in vaccinations. "All drugs have risks and side effects," says Bruce Thompson, a professor of health sciences at Swinburne University in Australia. Scientists are quick to point out that about a third of patients with COVID-19 also present with blood clots and that the risk of blood clots post-vaccination is lower than with the contraceptive pill.
In pausing or changing recommendations around the Vaxzevria or J&J vaccine, regulators are constantly weighing up the tiny risk of post-vaccination clots against the risk of problems resulting COVID-19 infection. As it stands, the benefits of vaccination still outweigh the risks in many countries where the pandemic is still raging out of control.
Updated April 14: Adds context to pauses, comment from J. Williams.

