Scientists create 'highway of death' for cancer
Instead of relying on drugs to kill tumors, Georgia Tech researchers engineer artificial pathways to lure malignant cells to their death, using a "Pied Piper" approach to treating cancer.
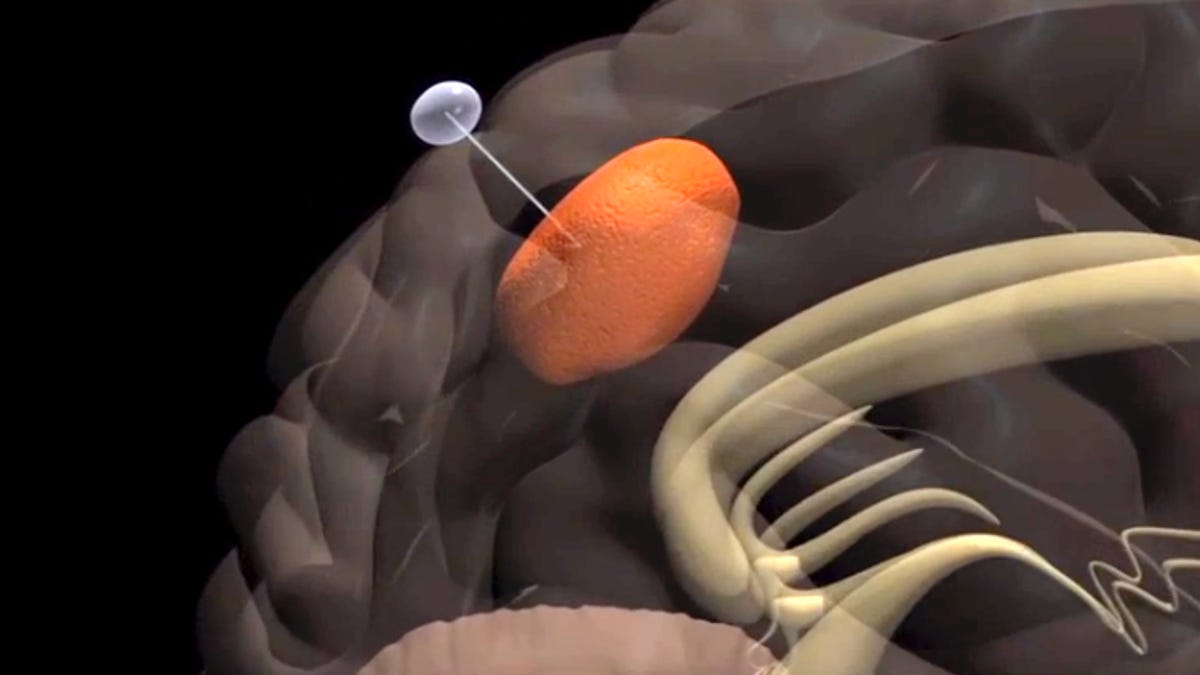
Brain tumors known as Glioblastoma multiform cancer (GBM) are a particularly insidious form of the disease because they just don't stay still. They travel through the brain by sliding along blood vessels and nerve passageways. This means that sometimes they move to parts of the brain where surgery is extremely difficult -- if not impossible -- or that even if the bulk of a tumor can be removed, chances are good its tendrils would still exist throughout the brain.
Scientists at Georgia Tech may have come up with a novel solution for this problem; though, it may be years before the technique can be used on humans. It involves creating artificial pathways along which cancer can travel. These pathways could route cancer to a more easily operable area, or even to a deadly drug located in a gel outside the body.
According to Ravi Bellamkonda, lead investigator and chair of the Wallace H. Coulter Department of Biomedical Engineering at Georgia Tech and Emory University, "the cancer cells normally latch onto ... natural structures and ride them like a monorail to other parts of the brain. By providing an attractive alternative fiber, we can efficiently move the tumors along a different path to a destination that we choose."
As reported Sunday in the journal Nature Materials, Bellamkonda and his team implanted nanofibers about half the size of a human hair in rat brains where GBMs were growing. The fibers were made from a polycaprolactone (PCL) polymer surrounded by a polyurethane carrier and mimicked the contours of the nerves and blood vessels cancer cells like to use as a biological route.
One end of a fiber was implanted into the tumor inside the brain and the other was inserted into a gel containing the drug cyclopamine (which is toxic to cancer cells) outside the brain. Sure enough, after 18 days, enough tumor cells had migrated along the fiber into the gel to shrink the tumor size 93 percent more in rats that received the treatment than in those that did not.
Not only does Bellamkonda think his technique could be used to relocate and/or destroy cancers, he says he believes it could be used to help people live with certain inoperable cancers as a chronic condition.
"If we can provide cancer an escape valve of these fibers, that may provide a way of maintaining slow-growing tumors such that, while they may be inoperable, people could live with the cancers because they are not growing," he said in a statement. "Perhaps with ideas like this, we may be able to live with cancer just as we live with diabetes or high blood pressure."
Many of today's methods for treating cancer focus on using drugs to kill tumors. The Georgia Tech team's approach was engineering-driven, thanks largely to Anjana Jain, the primary author of the study. She did her graduate work on biomaterials used for spinal cord regeneration. When she found herself working in Bellamkonda's lab as a postdoctoral fellow, she came up with the idea of using engineered materials to route cancer cells.
Path of least resistance
This approach allows cancer to be treated with a device rather than with chemicals, potentially saving the patient many debilitating side effects. "One attraction about the approach is that it is purely a device," Bellamkonda said. "There are no drugs entering the blood stream and circulating in the brain to harm healthy cells. Treating these cancers with minimally invasive films could be a lot less dangerous than deploying pharmaceutical chemicals."
Part of the innovation in the researcher's technique is that it's actually easier for tumors to move along the nanofibers than it is for them to take their normal routes, which require significant enzyme secretion as they invade healthy tissue. "Our idea was to give the tumor cells a path of least resistance, one that resembles the natural structures in the brain, but is attractive because it does not require the cancer cells to expend any more energy," Jain, now an assistant professor of biomedical engineering here at Worcester Polytechnic Institute, explained in a statement.
Extensive testing, which could take up to 10 years, still needs to be conducted before this technology can be approved for use in human patients. In the meantime, Bellamkonda says he'd like to see if the technology can be used to lure other cancers that like to travel along nerves and blood vessels using what he describes as the "Pied Piper" approach.

